Fulfilling, not ‘depressing’: Meet the volunteers and nurses who choose to provide end-of-life care
published by Channel News Asia Digital on July 22, 2023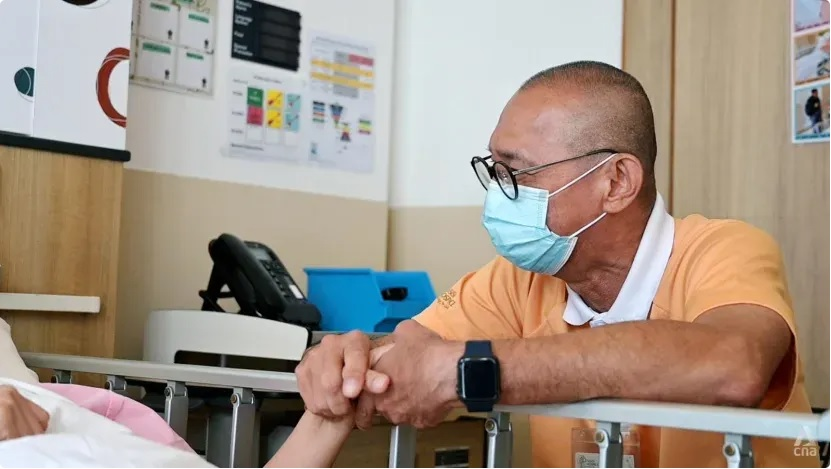
Dealing with death can be challenging for people providing palliative care. But these volunteers and healthcare workers tell CNA why it is a fulfilling job and how they cope with sadness.
SINGAPORE: When Dennis Hor volunteers at Assisi Hospice to provide companionship to end-of-life patients, he likens the experience to bidding farewell at an airport.
“The only difference,” he said, “is that I don’t really know when is the exact departure time.”
“I pray for them, I practice meditation while I’m with them, because during that final moment, most of them don’t respond anymore. But in my belief, they still can sense our love.”
Mr Hor is one of 46 volunteers who are part of the NODA@Assisi programme, which aims to support patients who don’t have anyone with them during the final stages of their lives. NODA stands for No One Dies Alone.
Some of these patients are single or are estranged from family members.
They are identified by their medical social workers to be considered for the NODA programme, which was started in 2014, said an Assisi Hospice spokesperson.
As Singapore’s population ages, efforts are being made to expand and improve palliative care – both in healthcare facilities and at home.
For instance, the Ministry of Health announced on Jul 1 that subsidies and MediShield Life claim limits will be raised to provide more financial help to palliative care patients.

Volunteers like Mr Hor play an important role in the palliative care ecosystem.
The 43-year-old, who is self-employed, said he joined NODA@Assisi because he was “concerned about the emotional impact” of losing his loved ones. He wanted to prepare himself to face the death of his loved ones as well as his own eventual passing.
“(Volunteering) gave me the strength to face the dying process head-on,” he said.
“I got the privilege to accompany two patients passing away and that experience really reshaped my knowledge about the dying process.”
Another volunteer, Paul Koh, was inspired to join the programme after witnessing how the nurses at Assisi Hospice comforted his sister-in-law during her final moments by tending to her, holding her hand and massaging her feet.
“It touched me and then I thought that one day, if I have the time (when I) retire, I think I should come and do some of these things,” the 69-year-old said.
Mr Koh said carrying out small errands for the patients, such as finding their spectacles and adjusting their pillows, is what brings them comfort.
Volunteers in the NODA programme are required to undergo basic volunteer carer training, which includes communication skills and familiarisation with inpatient duties.
They are equipped with practical clinical skills such as diaper changing, bed-sponging and assisting in the mobility of an ambulant patient.
Volunteers would also have to be familiar with where to seek emotional support for themselves if needed, said the Assisi spokesperson.
MAKING A DIFFERENCE
More than 20 healthcare institutions in Singapore provide palliative care across various settings.
At Alexandra Hospital’s palliative care ward, 22-year-old part-time basic care assistant Quraisyah Abdul Rahim was inspired to provide end-of-life care after witnessing the attention nurses gave when her late grandfather was hospitalised.
When asked about her decision to work in end-of-life care, Ms Quaraisyah explained: “I feel like I could make the patient’s quality of life better, as well as the family members’, because I understand how hard is it to go through this.”
Unlike Assisi Hospice, Alexandra Hospital sees patients who still require “clarification of their diagnosis” or condition and continue to receive active treatment, said Nurse Manager Pearlyn Ng.
The hospital’s palliative care programme, which was established in July 2019, also aims to facilitate direct admissions from community partners such as nursing homes, as well as train healthcare workers in palliative care.
Ms Quraisyah said she has received questions about why she chose to work in end-of-life care.
“One of my friends asked me something like, ‘Isn’t it depressing? You’re still young, are your parents okay with it?’”
But Ms Quraisyah said she finds fulfilment in being there for her patients and helping them create memories.
The care assistant recounts being part of a patient’s graduating photoshoot with her children.
“The medical social worker actually planned out a day with them so that before she passed on … the children have something to cherish and remember,” she said.
“I was able to actually get ready with her, like with her favourite clothes … I was able to help her with everything,” she told CNA with a smile.
“It’s just having to find the happy moments with them.”
Ms Quraisyah’s work in end-of-life care has strengthened her resolve to pursue a career in nursing.
She plans to apply to the Institute of Technical Education (ITE) for NITEC in Nursing at the end of the year.
It is a similar situation for Mr Hor and Mr Koh from the NODA programme, who said some of their friends struggle to understand why they volunteer to accompany terminally ill patients.
Mr Hor’s friends think his work could be inauspicious and wonder how he “can cope with that kind of sadness”.
But Mr Hor, who believes in the possibility of an afterlife, said thinking of death as an “evolution” rather than a loss helps him to manage the sadness that comes with the field of work.
He would also share with his family and friends the insights gained through his volunteering work in order to address the negative perceptions surrounding end-of-life care.
Ultimately, he hopes to inspire his loved ones to find their own ways to extend help to those in need.
Mr Koh said his friends questioned what he could possibly contribute when many patients are already bedridden and nearing the end of life. They also labelled his role as “sad and depressing”.
“I will explain to them … not all patients are bedridden, some are mobile, some are still alert, they just need (friends) to be around with them, holding hands, talking, accompany(ing) them during this difficult time,” he said.
Another common misconception about end-of-life care is that it signifies losing hope, said Alexandra Hospital’s Ms Ng.
“They think end-of-life care means that we are doing nothing,” she said, adding that it is crucial to reframe these misconceptions.
“There might not be (anymore) viable cancer treatment, but the care of our patient’s well-being and how they are to spend the rest of the time they have left still matters to us in palliative care,” Ms Ng said.
“Even when there’s no more available treatment … the caring never stops.”
COPING WITH EMOTIONS
While Mr Koh finds joy in providing companionship to terminally ill patients, he also acknowledges the sombre aspect of his role, with “mixed feelings” being present during their final moments.
“I’m saddened to lose a patient, but at the same time, I’m relieved that the patient’s suffering has come to an end … because sometimes the pain really is overwhelming,” he said.
It can be more difficult to cope if the patient is young.
“Young people, thirty-something, just pass on like that … usually they have problems with their family, that’s why NODA comes in,” he said.
“They don’t talk to their mother, father, you know, they have nobody to go to … and their partners are not responding to them”.
By finding solace in the knowledge that his companionship has brought comfort to the patient, Mr Koh said he is able to come to terms with loss and shift his focus towards the meaning of his work.
“I think being present at that moment is very important, it can make a big difference to the life of the patient,” he added.
For Ms Quraisyah, it can get quite challenging when a patient, with whom she has developed a rapport and cared for over a significant period, dies.
The care assistant said she tries not to focus so much on the deaths.
“I just think positive – that they are not suffering anymore and (are) passing on comfortably,” she told CNA.
“It’s a privilege that I actually get to spend the last moments with them,” she added.
“If I ever, like, feel sad, I always have my other nurses to talk (to).”
End-of-life caregivers may also encounter challenging situations during their shifts, especially when patients are struggling with intense emotions during the final stage of life and are not fully conscious.
Mr Hor once encountered an elderly patient who tried to strangle him out of anguish.
“That old lady keep calling ‘papa, papa’, so it’s very obvious at that moment she was looking for fatherly love, and I just act accordingly and try to comfort her,” he recounted.
“However, in the next moment, her emotions just turned the other way.
“She just show(ed) anguish, and then she raised up her hand and gave me a gesture to come closer to her, and next moment she kind of like want(ed) to strangle me,” he said.
“I think it made me ponder what she had gone (through) in her life … that she (has) such (an) intense emotional reaction in her final stage of life.”
It is important to acknowledge the feelings or emotions that come with loss, whether it is sadness, guilt or confusion, Ms Ng explained, highlighting the emotional stress involved in providing end-of-life care.
For Ms Ng, she would speak to her friends and colleagues to process these feelings.
“I think different people have different ways of doing it … I also know of friends who journal their feelings as well as do painting and art to release the tension,” she said.
“As a team, together with my other nurse leaders, we try to foster an environment that is supportive and we encourage nurses as well as care assistants to always voice out any opinions or concerns that they may have,” she added.
“Having a safe culture where people are able to speak up is important to sustain this work.”
“ONE CHANCE TO MAKE IT RIGHT”
So what drives these healthcare workers and volunteers despite the emotional challenges?
Ms Ng said she gets a sense of fulfilment helping to alleviate a person’s suffering and assist them in making the most of their remaining time.
“You just really move from focusing on treatment to focusing on the comfort and the well-being of the patient and (their) family and what they really want in life,” she told CNA.
“As the patients near their final moments, you know that they are comfortable, they are not in distress, they are not in pain, they are not breathless,” she added.
“We only have one chance to make it right for these patients who are passing on, and the memory of their loved ones passing will forever be etched in the memories of the family members.”
After nearly two years of working in end-of-life care, Ms Quraisyah said her outlook towards family and friends has shifted. She now devotes more time to being with her loved ones.
“Also, I always remind myself not to get scared to try new things because you never know – maybe I don’t have the chance to do it again if I don’t,” she added.
Ms Ng similarly said the job has made her more appreciative of each day.
“I learned not to take things for granted, as well as to be more present in each interaction that we have, be it with friends or family – especially family since those are the people whom we always take for granted,” she said.
For Mr Koh, the people he has met through the volunteering experience have helped him understand their various concerns and anxieties about the end of life.
“That taught me to be more patient, more loving,” he said. “Don’t sweat the small stuff … and help whenever possible.”

