Make-believe outings and virtual pet therapy: Hospices get creative to bring patients joy during circuit breaker
published by Channel New Asia Digital on May 24, 2020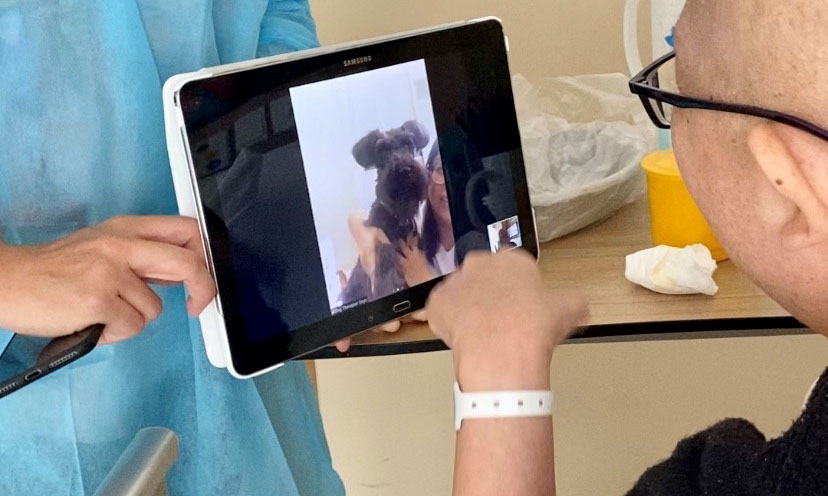
SINGAPORE: Going out for trips to Haw Par Villa or Little India were long the norm for patients of HCA Hospice Care.
But with COVID-19 “circuit breaker” restrictions in place, Polly Lim needed to use a little more imagination if she wanted to keep her patients’ spirits up.
After hearing some of them complain about not being able to go out, she thought – if they cannot venture out, why not bring the world in?
Ms Lim decided to organise a retro-themed party because the patients often reminisce about the past.
So on Apr 17, the hospice’s day care team took them on an “excursion” to the past. Old-school printouts of bus tickets were issued, which the patients used to enter the day care centre. The place was decorated with black-and-white posters of celebrities from the 30s and 40s.
Employees put up a show on the seven steps of hand washing, performed to the tune of Saturday Night Fever. A few patients later joined them on the dance floor.
Lunch was dim sum – served to them in pushcarts.
The rest of the afternoon was spent lounging in an area that had been converted into a “beauty parlour”. The hospice team gave them manicures, foot spas, facial, and a shave for the men. A colleague, dressed up as Charlie Chaplin, made an appearance to hand out some snacks.
“There was a lot of laughter, a lot of smiles. Some of them are still talking about it today,” said Ms Lim, HCA’s day hospice assistant supervisor. “I know they miss our outings a lot. My team and I just wanted to do our best to add (life) to their days.”
These were just some of the ideas hospices have come up with to bring cheer to terminally ill patients, to help them cope amid circuit breaker measures such as restrictions on group activities and the number of visitors allowed.
At Assisi Hospice, an employee dresses up every Tuesday as a postman delivering origami flowers and cards with well-wishes from volunteers.

At Dover Park Hospice, occupational therapists sometimes offer gardening tools or dry herbs to patients who miss the outdoors. Two weeks ago, an elderly man who loves gardening received a bag of soil and some pots.
“The patient transformed. He was no longer his tired, lethargic self,” said Ms Grace Sim, a senior principal occupational therapist at Dover Park.
“There are limitations to what we can do to enhance patients’ quality of life, but we’re still trying our best to bring a sense of normalcy and help them live their last days to the fullest.”
Giving patients therapeutic objects is something staff members had been doing for those who are bed bound. But they are now also doing so more frequently for other patients, since they are not allowed to stroll around the grounds of the hospice as part of circuit breaker measures.
THERAPY THROUGH TECHNOLOGY
With the circuit breaker in play, hospices have had to quickly embrace technology.
Staff members at all three hospices have been kept busy setting up video calls between patients and loved ones who are unable to visit, as well as with volunteers who are now not allowed to go to the hospices. This means employees at end-of-life facilities have also had to take over roles that were performed by volunteers.
Dover Park’s Ms Sim recently set up an online file sharing system for volunteers to send resources they think will keep the patients busy, such as soft copies of sudoku puzzles and videos of dialect songs.
This saves the therapists a lot of time, she said. “I can’t imagine my staff trying to sit and Google (for these materials).”
At Assisi, pet therapy has gone online. Their therapy dog, which used to stop by the hospice once a week, now makes an appearance through a tablet from its home with its owner.
Although none of these virtual initiatives can match up to the connection physical companionship provides, hospice representatives said patients have mostly been appreciative of their efforts.
Hospices provide mainly three types of services – in-patient care, home care which involves healthcare workers visiting the patients at their houses, as well as day care where the patients drop by the hospice.
With hospitals trying to free up more beds for COVID-19 cases, hospices have had to take in more of their terminally ill patients, tapping telemedicine in the meantime to cope with the higher workload – albeit cautiously.
Since the coronavirus outbreak, HCA has more than doubled it home hospice care cases from 150 in February to more than 300 in April, said Ms Ng Wan Ru, a home hospice nurse.
Most of them are hospital referrals, while the rest are former day hospice patients who had to be transferred out when HCA reduced its day hospice intake from 60 to 25 to comply with safe distancing rules.
“If we did do video consults, it used to be unofficial – the patient just wants to check on a pain point or issue briefly, and we can ascertain whether we need to be there physically,” said Ms Ng.
But several weeks ago, her hospice formally introduced a telemedicine system pilot, she said, putting willing and non-urgent cases on their video consultation list.
These are Internet-savvy patients they must have seen before whose conditions are identified as stable enough to warrant less frequent home visits.
“We have (a) strict criteria,” she stressed. “They mustn’t be in a lot of pain, and they don’t need a physical examination for us to be confident to identify what the causes of their discomfort are.”
Like Ms Ng, Dover Park’s chief executive Timothy Liu was quick to emphasise that there is an official guideline hospices follow when it comes to telemedicine. His organisation, which also provides home hospice care, employs standards similar to HCA’s.
Video consultations can never replace face to face visits, said Ms Ng, who also explained that some patents clam up during video calls. “As a healthcare professional, you need to see and feel for yourself at some point what the patient is going through to make a serious judgment call.”
At the end of the day, relying on technology is a balancing act in an industry that is as much about emotional care as it is about physical health.
“When a patient or caregiver cries over the phone or the screen, you are not able to give them a tissue, hold their hand, give them a pat on their back,” said Ms Koh Yuqi, a social worker who supports HCA’s home hospice patients.
“All these are very small but significant acts.”
SAYING GOODBYE HAS BECOME A DIFFICULT ISSUE
In palliative care, treating the dying is not just about managing their pain or making a last-ditch attempt to get them well again, said hospice professionals.
“We are looking at what we call a good death,” said Mr Liu. “How a person and their family members are able to resolve many of the worldly conflicts and tensions (and) have some closure.”
In a world of COVID-19, fulfilling some of the patients’ last wishes has become tougher. Some want to seek forgiveness, others just want to spend as much time with as many family members as they can.
But with both home and hospice visits limited by safe distancing rules, hospice employees have had to help them make do with the present circumstances.
“They would ask: ‘Am I breaking the law if my daughter visits?’,” said HCA’s Ms Koh. “And you know this is so important to them because time is very precious.”
“They want to see their loved ones for the final time, share their last words, express words of gratitude and appreciation, seek forgiveness, and say goodbye to the people that meant the world to them.”
“It is a challenge with all this going on,” she said. She would encourage those whose loved ones are unable or afraid to visit to drop a video or phone call, pen a letter or make a piece of artwork to express their feelings.
Most are open to it, but some insist that reconciliation and closeness can only be forged through physical contact, she said.
Family members have also shared their personal regrets with hospice workers.
“What has been difficult has been the conversations with the family members,” said Cheong Ee May, the head of social work and psychosocial services at Dover Park, which like Assisi, has required its live-in patients to nominate four designated visitors during the circuit breaker. At any time, only two can drop by.
“If they are part of a big family, some of them may never get to say goodbye physically because they are not on the list of designated visitors,” she said.
“They can’t touch him for the last time, give him the last hug, or tell him face to face how much I love him. If the patient’s in a blurry state, they may not recognise the person on the phone.”
Funeral rites have also become another issue, they said, given the limit of 10 attendees in a room at any time. “The family members lament about the coldness of the send-off ritual,” said Ms Koh.
“I have seen big families who are very close-knit, it’s very painful for them because they have to select who can come, and who can’t.”
PHYSICAL, MENTAL TOLL ON HOSPICE EMPLOYEES
The circuit breaker and the growing number of patients have also taken a toll on hospice employees.
Assisi’s in-patient admissions, for instance, have increased by 25 per cent between January and April this year, compared to the same period in 2019, said Juliet Ng, the hospice’s communications and community engagement head.
The hospice has been forced to recall some of their nurses on their days off or who are on their annual leave.
HCA’s Ms Ng said she has had to pack more calls and visits within her eight-hour shifts.
Wearing protective gear the entire day in Singapore’s weather is also no fun for home care aides, who are drenched in sweat after the first hour of work. Neither is eating lunch at a corner of a staircase landing at an HDB block, or skipping lunch altogether.
Most of all, it is the mental and emotional drain that has grown during this period, the hospices’ representative said.
Colleagues can no longer sit down and talk to one another in person to decompress after a hard day’s work. When they get home, they minimise contact with family members to reduce the potential risk – should they get COVID-19 – of passing on the virus to their vulnerable patients.
Every day, they face the task of reminding patients that the circuit breaker has not ended.
“The elderly (patients) ask you everyday: ‘Have they changed the restriction?’ And you have to explain to them ‘not yet’,” said Assisi’s Ms Ng.
“It really bothers us, that’s why we have to constantly come up with ways to (create some form of human connection) for our patients. Technology helps, but its never enough,” she added.
“You feel very bad. You feel their yearning to see their loved ones. (But there’s just) no choice.”
If there is one silver lining for these healthcare staff, it is the opportunity to meet more of their home care patients’ family members, given that most people are home during the circuit breaker period.
“The beautiful part about the COVID (period) is that we have a lot of families around (and) we get to see a lot of families whom we have never met before,” said HCA’s Ms Ng.
“We witness a lot of pain and suffering … but at the same time we are so privileged because we (get to) witness so much love, strength and patience, learn so much about resilience from our patients and families,” she said.
Some patients also appreciate being in the presence of family more often.
“I had one patient who told me she now she gets to enjoy having her grandkids around her all the time, watching them run around, play with their pet turtle,” Ms Ng said.
She recalled another patient whose words have stayed with her since. “(It) was something so simple: ‘I’m happier during this COVID period’,” she said.
“It’s simple, it’s direct, but it just show that what we cherish most is that human connectedness.”
Click Here to view full article

